Integrated EHR Billing
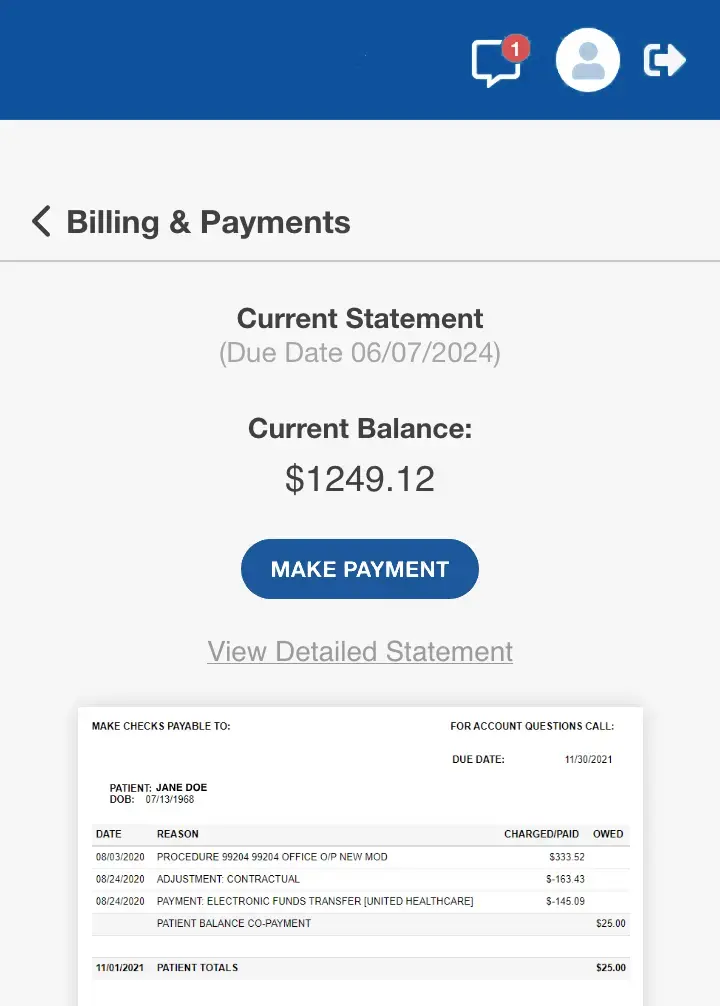
Billing Built for the Complexity of Modern Healthcare
Revenue cycle management should not feel disconnected from patient care. Healthcare organizations manage a constant flow of visits, procedures, diagnostics, follow-up care, documentation requirements, and payer expectations—where even small workflow gaps can delay reimbursement or create operational strain.
WRS Health keeps billing tightly connected to clinical and operational workflows so documentation, coding, charges, and claims move together within one platform.
Whether providers are managing routine visits, specialty care, procedures, chronic conditions, or multi-location operations, WRS Health helps practices maintain stronger alignment between care delivery and financial performance.
Schedule Free ConsultationIntelligent Workflows That Help Protect Revenue
Modern healthcare billing involves far more than claim submission. Documentation accuracy, coding consistency, eligibility verification, and operational follow-through all impact reimbursement outcomes.
WRS Health includes intelligent tools that support billing workflows from the moment documentation begins.
Connected Revenue Cycle Support Includes:
- Real-time coding guidance that helps reduce missed charges
- A proprietary Billing Rules Engine that flags potential issues before submission
- Documentation support aligned to visits, procedures, diagnostics, and treatment workflows
- Automated safeguards that help reduce audit and compliance risk
- Connected workflows that reduce delays between care delivery and claim submission
The result is cleaner claims, faster processing, improved visibility, and more predictable reimbursement workflows.

Faster Intake Supports Cleaner Claims
Intelligent intake workflows capture demographics, insurance information, consent forms, and visit-related details before or during the encounter so claims begin with more complete information.
Practices spend less time chasing missing data after appointments while reducing front-desk bottlenecks and downstream billing corrections.
The result is:
- Cleaner claims
- Faster submission workflows
- Reduced administrative friction
- Improved operational consistency
- Stronger cash flow visibility
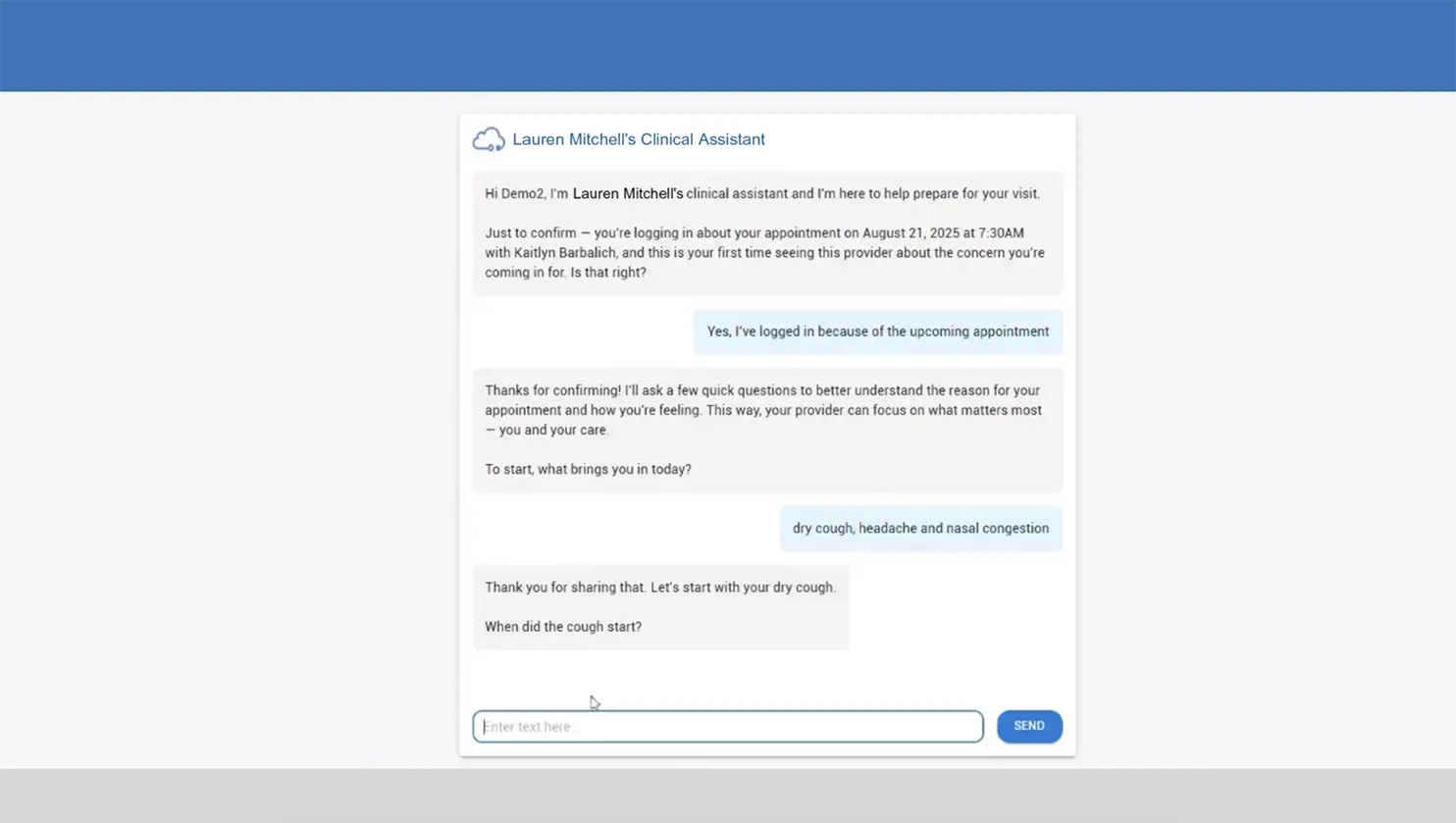
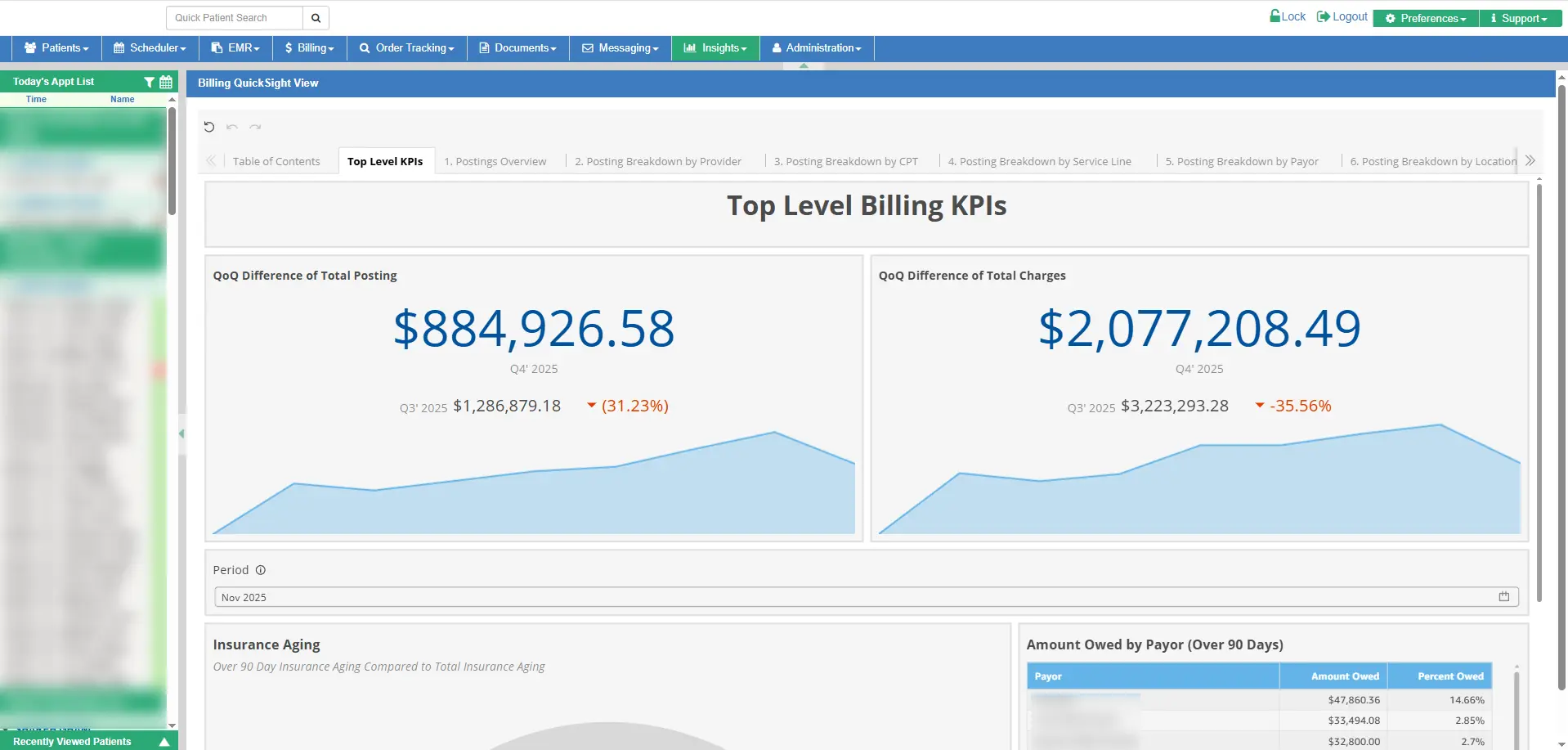
Revenue Cycle Workflows That Operate in the Background
The best billing workflows reduce operational burden instead of creating additional work for providers and staff.
WRS Health automates eligibility checks, coding support, claim preparation workflows, and billing safeguards behind the scenes so teams can stay focused on patient care and operational efficiency.
With scheduling, documentation, intake, and billing connected inside one platform, practices experience:
- Fewer billing disruptions
- More consistent workflows
- Faster reimbursement cycles
- Improved visibility into financial performance
- Reduced manual administrative effort
A Complete Revenue Cycle Management Solution
WRS Health combines billing, coding support, workflow automation, AI-powered safeguards, and specialty-aware operational workflows within one connected platform.
The system supports:
- Independent practices
- Multi-location provider organizations
- Specialty-focused groups
- Procedure-driven workflows
- Growing healthcare organizations with operational complexity
Practices benefit from:
- Documentation tied directly to coding and billing workflows
- Automated operational processes with fewer delays
- Lower denial rates and improved collections visibility
- Streamlined charge capture across visits, procedures, and diagnostics
- Connected reporting and financial oversight
Spend less time correcting billing issues and more time supporting patient care and practice growth.
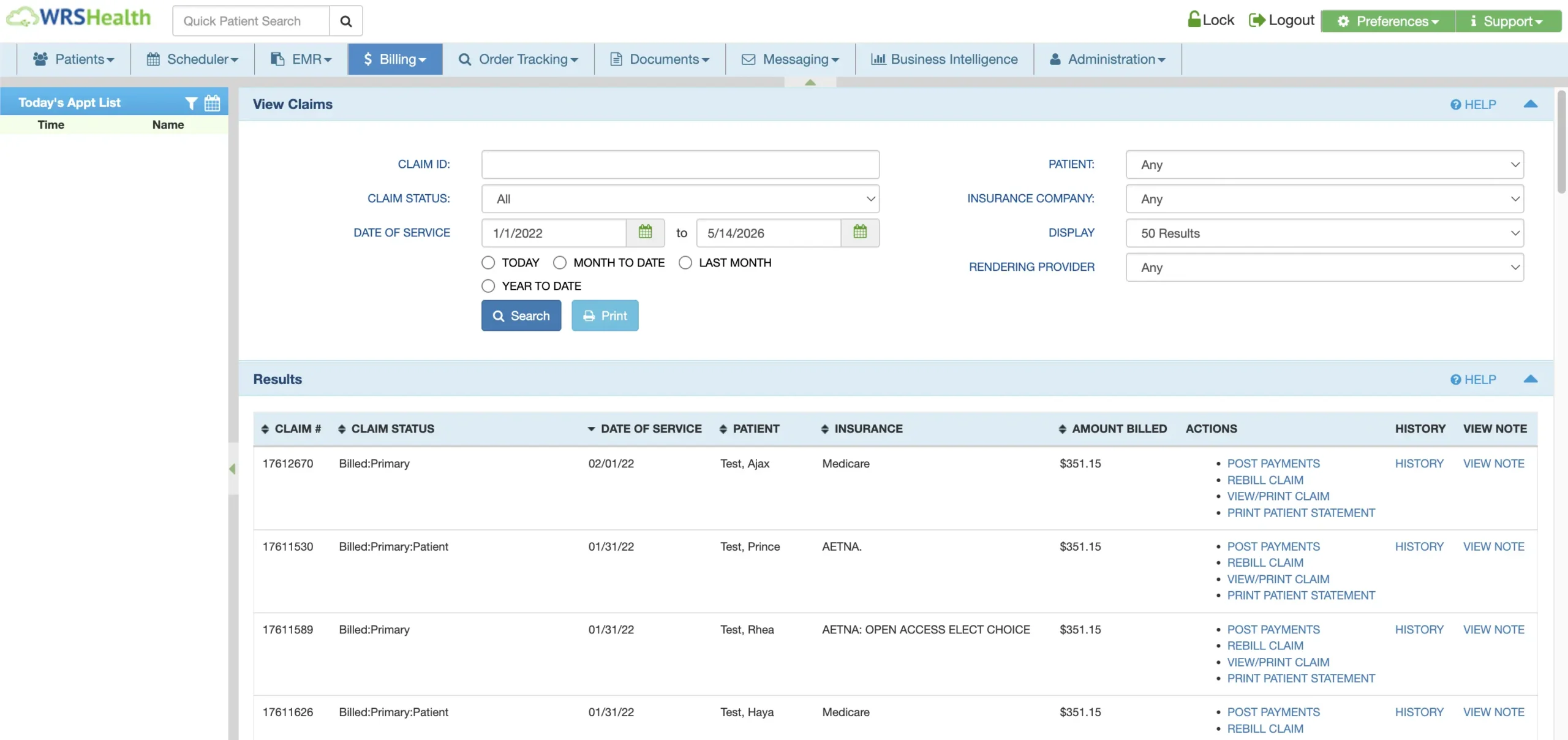
Need Additional Billing Support?
WRS Health also offers managed billing services supported by experienced healthcare revenue cycle specialists.
From claim submission and denial management to follow-up workflows and collections optimization, our billing team works alongside your organization to help maximize reimbursement while reducing administrative burden.
Explore Our Billing ServicesLet’s Get The Conversation Started
Fill out the form below to request a personalized demo.
 QUICK CHARTING
QUICK CHARTING NOTE
NOTE MEDICATION
MEDICATION PATIENT
PATIENT BILLING
BILLING RISK
RISK MARKETING
MARKETING MIPS
MIPS